Mid-upper-arm circumference as a screening measure for identifying children with elevated body mass index: a study for Pakistan
Article information
Abstract
Purpose
Mid-upper-arm circumference (MUAC) is considered an alternative screening method for obesity. The aims of this investigation were to examine the ability of MUAC to correctly identify children with elevated body mass index (BMI) and to determine the best MUAC cutoff point for identification of children with high BMI.
Methods
Anthropometric measurements (height, weight, and MUAC) from a cross-sectional sample of 7,921 Pakistani children aged 5–14 years were analyzed. Pearson correlation coefficients between MUAC and other anthropometric measurements were calculated. Receiver operating characteristic curve analysis was used to determine the optimal MUAC cutoff point for identifying children with high BMI.
Results
Among 7,921 children, the mean (±standard deviation) age, BMI, and MUAC were 10.00 (±2.86 years), 16.16 (±2.66 kg/m2), and 17.73 (±2.59 cm), respectively. The MUAC had a strong positive correlation with BMI. The optimal MUAC cutoff points indicating elevated BMI in boys ranged from 16.76 to 22.73, while the corresponding values in girls ranged from 16.38 to 20.57.
Conclusion
MUAC may be used as a simple indicator of overweight/obesity in children, with reasonable accuracy in clinical settings.
Introduction
In the recent years, obesity prevalence in children and adults has been well documented. Children during childhood age, usually taking high energy diet and having low physical activity may get trapped by obesity.12) Childhood obesity has therefore now become global pandemic. Nearly 10% of the school-going children in the world are being reported as overweight and one quarter of these are being obese.34) Available evidences consistently report that these alarming patterns are also emerging in the developing countries including Pakistan.567) A study conducted by Mushtaq et al.8) has shown that the prevalence of overweight and obesity in the Pakistani primary school children is about 17% and 7.5%, respectively.
Body mass index (BMI) is the most extensive and internationally recommended criterion used for defining overweight and obesity in both children and adults.9) Despite the popularity and ease to use, it has fewer limitations.10) Some studies have also demonstrated the value of waist circumference, waist-to-hip ratio, and waist-to-height ratio as a measure of central obesity.1112) However, these all measurements have some practical barriers in clinical measurements; clothing is one the major disturbing factors during measurements.13)
Recently, mid-upper-arm circumference (MUAC) has been proposed as another important indicator of obesity in children. Measurements of MUAC have long been known to reflect changes in human body weight, and the major determinants of MUAC, arm muscle and subcutaneous fat, are both important determinants of survival in starvation.14) In 2003, de Almeida et al.15) for the first time suggested that MUAC was an alternative screening method to be used as a potential proxy for obesity in children. After that, it was proved by Mazıcıoğlu et al.16) in the Turkish children, aged 6–17 years. Measurement of MUAC is an easy, quick and inexpensive activity and now various pediatric investigators171819) have attempted to use it for screening of overweight and obesity in children and adolescents.
In Pakistan, there is a dearth of research on the potential use of MUAC as a screening tool for overweight and obesity of children or for other clinical practices. Considering such negotiable gap, we carried out the present study with the following objectives: (1) to examine the ability whether MUAC can correctly identify children with elevated BMI and (2) to determine the sex-specific and age-specific best cutoff values for MUAC that would identify overweight/obese children.
Materials and methods
1. Study population and design
A population based cross-sectional study sample of age 2 years and above was collected from Pakistan's most populated province viz. Punjab. Three major administrative cities Multan, Lahore and Rawalpindi and the capital city, Islamabad were purposively selected. Multan is the most populous city of south Punjab and is located at the central part on Pakistan's map. Population in this city has its own climatic, social and ethnic characteristics. Lahore, a metropolis, is the capital of province Punjab with different ethnic groups. Rawalpindi and Islamabad are 2 adjacent cities namely called twins cities and Islamabad being the capital of Pakistan also has multiethnic populations.20) The present study was a part of a large study of different anthropometric measures for different age groups. The sample for this article is based on 7,921 children aged 5–14 years in order to identify their overweight and obesity status using MUAC and BMI data. The data were collected from different public and private schools (primary, secondary, and higher secondary) and from different public places. The complete list of schools (comprised of primary, secondary, and higher secondary) of the respective cities was taken from Punjab Department of Education (Schools). Random sampling was used for school selection. A date for an educational institute visit was scheduled. The permission was granted from the school's head and if any school's administration refused to participate, next school was selected from the respective list. From each selected school, a list of all classes of each grade was obtained from the school's head and one class of each grade was randomly selected. From each of the selected class, minimum 20 students included in the study by using nonprobability convenient sampling. This was done after some discussion with the concerned school's head based on class schedules.
All the healthy children aged 5–14 years, who were not taking any medication and having not any physical disability were included in the study. All the children who did not meet these criteria were excluded. Furthermore, we also tried to ensure that our study sample could cover all the socio-demographic (economic) class of people and ethnicities of Pakistan.
2. Data collection and ethical concern
Data collection activity was completed during March to June, 2016 by three well-trained data collection teams. Each team was consisted of 3 members, supervised by the principal investigator. The required information was taken through a self-administered questionnaire, comprised of demographic information section and measurement section. The demographic section contained the information like gender status (boys/girls); age (rounded to next year) of children recorded from school register with the assistance of class teacher. The measurement section contained the information about the anthropometric measurements.
After complete explanation of the objectives of the study, a written consent from each school's head and a verbal consent was taken from each child. They had the right to voluntarily participate in or withdraw at any time from the study. The study was approved by the departmental ethics committee of Bahauddin Zakariya University, Multan.
3. Anthropometric measures
The MUAC and other anthropometric measurements such as height and weight were taken from each participant, using standard techniques21) as under: height (cm) without shoes was taken on a stadiometer (Seca: SCA217), and weight (kg) in light cloths was measured using weighing machine (Westpoint WF7009). The MUAC (cm) was measured using a nonelastic plastic tape at the midway between the olecranon and acromion process on the upper left arm. During these measurements, the subject was in comfortable standing position and asked to look straight ahead with shoulders in normal position. Subject's arm was also straightened. The tape was wrapped around the straightened arm at the mid of upper arm and the tape was inspected to ensure it was neither too tight nor too normal.
4. Statistical tools
Since the LMS method was used to construct the USCDC 2000 growth curves, we also used the LMS method to obtain z score in the present study. The LMS method summarizes the distribution of BMI by age and sex in terms of 3 curves namely called L (lambda), M (mu) and S (sigma).22) The L curve expresses the skewness of the BMI distribution in terms of the Box-Cox power transformation needed to transform the data to near normality. The M and S curves express the median BMI by age and coefficient of variation of BMI, respectively. The z score for BMI measurement (X) was calculated as: 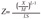 if L≠0 or
if L≠0 or 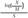 if L=0, where the values L, M, and S are for child's age and sex.22) The World Health Organization (WHO) z scores cutoffs were used to define overweight and obesity status of a subject which were: using BMI-for-age z scores; overweight (>+1SD i.e., z score >1) and obesity (>+2SD i.e., z score >2).2324) Means and standard deviation of each numerical variables were reported for both sexes. Two-sample independent t test was used to check their means comparison and Pearson correlation was used to investigate the correlation between MUAC and other anthropometric measurements. Odds ratios (ORs) were also computed to determine the strength of associations. To find the optimal cutoff points of MUAC for predicting how well they could separate the normal subjects from having elevated BMI (i.e., BMI>+1SD; overweight including obesity), the receiver operating characteristic (ROC) curve analysis was used. The optimal cutoff point of MUAC was defined as a value which represented the maximum sum of sensitivity and specificity in each sex, stratified by age. An MUAC value with highest Youden index was chosen for cutoff point. The diagnostic test, area under the curve (AUC) was used as an indicator of overall accuracy of using the MUAC cutoff point to discriminate subjects with or without elevated BMI. Accordingly, if an AUC was 0.65 to 1.00 and 0.50 to 0.65, the test was considered ‘highly accurate’ and ‘moderately accurate’, respectively.2526) The likelihood ratios (positive [LRP] and negative [LRN]) for MUAC that were predictive of overweight and obesity were computed for each age and sex. The [LRP] of a positive test result is obtained by dividing sensitivity to the 1-specificity and it tells how much the odds of a disease increases when a test is positive. Conversely, the [LRN] is obtained by dividing 1-senseitivity to the specificity and it tells how much the odds of a disease decreases when a test is negative.27)
if L=0, where the values L, M, and S are for child's age and sex.22) The World Health Organization (WHO) z scores cutoffs were used to define overweight and obesity status of a subject which were: using BMI-for-age z scores; overweight (>+1SD i.e., z score >1) and obesity (>+2SD i.e., z score >2).2324) Means and standard deviation of each numerical variables were reported for both sexes. Two-sample independent t test was used to check their means comparison and Pearson correlation was used to investigate the correlation between MUAC and other anthropometric measurements. Odds ratios (ORs) were also computed to determine the strength of associations. To find the optimal cutoff points of MUAC for predicting how well they could separate the normal subjects from having elevated BMI (i.e., BMI>+1SD; overweight including obesity), the receiver operating characteristic (ROC) curve analysis was used. The optimal cutoff point of MUAC was defined as a value which represented the maximum sum of sensitivity and specificity in each sex, stratified by age. An MUAC value with highest Youden index was chosen for cutoff point. The diagnostic test, area under the curve (AUC) was used as an indicator of overall accuracy of using the MUAC cutoff point to discriminate subjects with or without elevated BMI. Accordingly, if an AUC was 0.65 to 1.00 and 0.50 to 0.65, the test was considered ‘highly accurate’ and ‘moderately accurate’, respectively.2526) The likelihood ratios (positive [LRP] and negative [LRN]) for MUAC that were predictive of overweight and obesity were computed for each age and sex. The [LRP] of a positive test result is obtained by dividing sensitivity to the 1-specificity and it tells how much the odds of a disease increases when a test is positive. Conversely, the [LRN] is obtained by dividing 1-senseitivity to the specificity and it tells how much the odds of a disease decreases when a test is negative.27)
The software, IBM SPSS Statistics ver. 21.0 (IBM Co., Armonk, NY, USA) was used for all the statistical analyses and a P value <0.05 was considered as statistically significant in the analyses.
Results
1. Participant characteristics
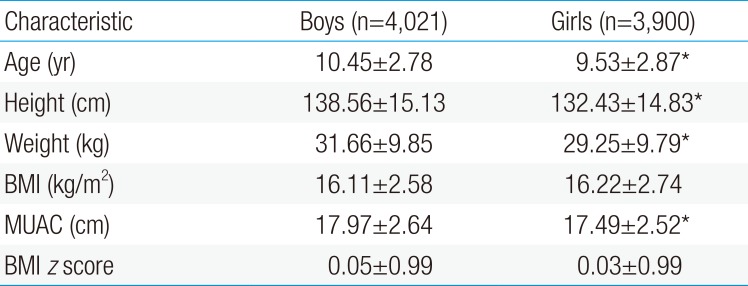
A total of 7,921 (4,021 boys and 3,900 girls) children, aged 5–14 years, were included in the study. Mostly, children (59.5%) were belonged to the 10–14 years age-group and 40.5% were aged between 5 and 9 years. The mean (±SD) of age, BMI, and MUAC of the total subject were 10.00 (±2.86) years, 16.16 (±2.66) kg/m2, and 17.73 (±2.59) cm, respectively. Overweight and obesity prevalence in all the subjects were 16.0% and 3.3%, respectively. Higher prevalence of obesity was observed among boys than girls (boys vs. girls: 3.6% vs. 2.9%). However, overweight prevalence among both boys and girls were similar (16.0%).
The descriptive statistics of age and anthropometric characteristics by sex were described in Table 1. Among the variables analyzed, mean age, height, weight and MUAC in boys were significantly higher than in girls. However, the BMI z score for boys and girls (0.05±0.99 vs. 0.03±0.99, P>0.05) were not significantly different. The normative values of MUAC for both boys and girls, according to age are presented in Table 2.
2. Correlation between MUAC and other anthropometric characteristics
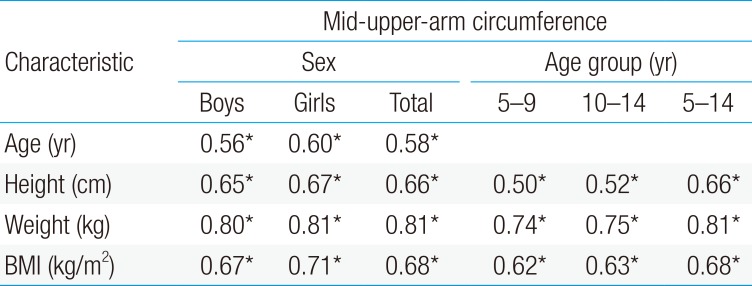
The values of correlation coefficient of MUAC with other anthropometric characteristics by sex and age-groups were displayed in Table 3. It was found that the MUAC had a strong significant positive correlation with age, height, weight, and BMI (P<0.001) in both sexes as well as in all the subjects studied. The results for correlation between MUAC and all other anthropometric characteristics by age-groups had also the same pattern. On the other hand, modeling in different situations of associations also showed that MUAC had a statistically significant positive association with overweight/obesity. The crude ORs and adjusted ORs for overweight/obesity were respectively, 1.57 (95% confidence interval [CI], 1.53–1.61) and 1.98 (95% CI, 1.91–2.06).
3. Association of MUAC with obesity (ROC analysis)
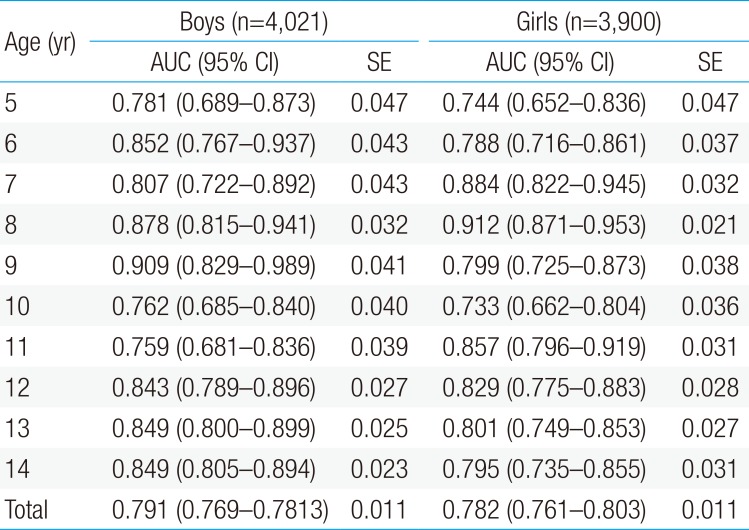
The ability of MUAC to accurately define elevated BMI was assessed by the results of AUC for both genders across all age groups. Table 4 presents the ‘highly accurate’ level of MUAC i.e., AUC >0.65 for identifying elevated BMI of both boys and girls (AUC: approximately 0.733–0.909 across all ages). For the children aged 5–9 years, the AUC for boys and girls were 0.828 (95% CI, 0.790–0.867) and 0.819 (95% CI, 0.787–0.851), respectively. On the other side, for the children of 10–14 years, the AUC for boys and girls were 0.804 (95% CI, 0.777–0.831) and 0.792 (95% CI, 0.764–0.820), respectively.

Area under the curve (AUC) for detection of overweight/obesity based on the mid-upper-arm circumference
Based on the ROC analysis, sensitivities, specificities and cutoff points for each age-group by sex were presented in Table 5. Considering all the children included in the study, the cutoff points of MUAC that identified elevated BMI in boys and girls were 19.17 cm and 17.90 cm for boys and girls, respectively. The likelihood ratios for each cutoff point were also shown. For example, LRP for a 14-year-old boy with MUAC >22.73 cm indicates that he is 6.27 times more likely to be overweight or obese than a 14-year-old boy with MUAC values below this cut point.
Discussion
In Pakistan, present study was the first of its kind that was discussing the use of MUAC measurement as a simple screening tool for identifying children with elevated BMI. Obesity prevalence greatly varied in different populations of the world. Our study results, based on the MUAC, showed that obesity prevalence was lower in the Pakistani children (boys vs. girls: 3.6% vs. 2.9%) when compared with the Jordanian children28) aged 6–12 years (5.6% for boys and 5.5% for girls) and with the Saudi Arabian children29) (5.98% for boys and 6.74% for girls). A study about the Chinese children aged 7–12 years reported obesity ranged from 3.9% to 5.3% among boys and 0.8% to 3.0% among girls of different age groups.30) It was noted that the Arabian girls were more obese than boys but our findings were consistent with those reported for the Jordanian and Chinese children.
Benítez Brito et al.31) also reported the MUAC to be a strong significant predictor of BMI (R2=0.61). In the study of Han children, Lu et al.17) reported that the MUAC had a significant correlation with age and other anthropometric variables for both boys and girls. We also had the similar findings in our study.
In our study, the results for AUC values between 75% and 90% in various age-groups which were consistent with the robust diagnostic performance1718) and suggested that measurement of MUAC could perform more accurate to discriminate children with or without elevated BMI. Furthermore, the cutoff point of MUAC to identify children with elevated BMI in different age-groups was between 16.76–22.73 and 16.38–20.57 for boys and girls, respectively. These findings suggested an action level lower than as compared to a previous study.17) Our MUAC cutoff values were also lower than the values reported by Mazıcıoğlu et al.16) This difference may be explained due to the ethnic variation and age range (i.e., 5–14 years in the present study).
In the earlier studies,1617) the MUAC was reported to be a substitute and an important indicator of obesity. However, systematic monitoring of MUAC in each country and their cutoff values have not been yet established.
The primary limitation of the study was the lack of ethnic variation. More analysis is required in this regard. Moreover, the inherent variability in anthropometric measurement could not be taken into account.
In conclusion, our study results revealed that MUAC showed a good correlation with BMI and MUAC therefore could be proposed as a simple and easy index to discriminate children with elevated BMI. However, more studies in children and young adults should be carried out to evaluate the usefulness of MUAC as an index of adiposity.
Notes
Conflicts of interest: No potential conflict of interest relevant to this article was reported.