- Review Article
- Nutrition
- Dietary fiber in pediatric gastrointestinal health: a narrative review of evidence and challenges
- Rohit Das, Bipashna Thatal, Buddhiman Tamang
- Clin Exp Pediatr. 2026;69(6):456-472. Published online May 27, 2026
-
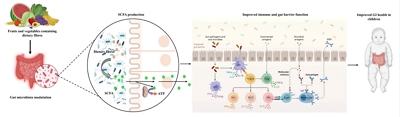
Dietary fiber plays a critical role in pediatric gastrointestinal health by modulating gut microbiota, improving bowel function, and supporting immune development. Evidence consistently supports its benefit in functional constipation, while effects on abdominal pain, inflammatory bowel disease, and irritable bowel syndrome remain variable due to differences in fiber type, dosage, and study design. Clinically, fiber should be used as an adjunct therapy within individualized dietary and behavioral management strategies for children.
- Allergy
- Update on pediatric allergic rhinitis: narrative review based on guideline updates
- Jung Yeon Shim
- Clin Exp Pediatr. 2026;69(6):473-483. Published online May 28, 2026
-
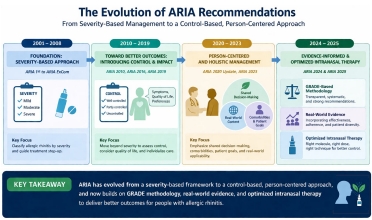
Intranasal corticosteroids remain the cornerstone treatment for moderate to severe allergic rhinitis. The 2024–2025 Allergic Rhinitis and its Impact on Asthma guideline update suggests that fixed intranasal antihistamine–intranasal corticosteroid combinations may provide greater symptom control in allergic rhinitis than either agent alone. A control-based patient-centered approach that incorporates real-world evidence is essential for optimizing treatment outcomes in children.
- Editorial
- Cardiology
- Beyond morphometry: the atrial septal defect pressure gradient as a dynamic predictor of mitral valve growth in borderline left hearts
- Han Ki Park
- Clin Exp Pediatr. 2026;69(6):484-485. Published online May 27, 2026
-
Traditional morphometric scores often fail to predict the success of biventricular repair of borderline left hearts. Wang et al. demonstrated that a low atrial septal defect (ASD) pressure gradient is a critical functional predictor of mitral valve growth. By integrating ASD hemodynamics with anatomical data, clinicians can better identify candidates for biventricular repair, proving that the "grey zone" is narrower than previously thought and improving outcomes for vulnerable neonates.
- Original Article
- Endocrinology
- Thyroid peroxidase gene variants and susceptibility to congenital hypothyroidism and autoimmune thyroid disease among Egyptian pediatric cohort
- Hala M. Sakhr, Mohammed H. Hassan, Esraa Abbass Abdallah, Amira Mahmoud Ewis, Mohamed Hesham Mohamed, Shymaa Gaber Rizk
- Clin Exp Pediatr. 2026;69(6):486-496. Published online March 26, 2026
-
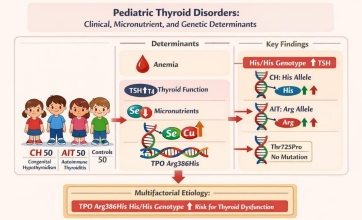
Question: Which factors influence pediatric thyroid disorder susceptibility and severity?
Finding: Anemia, selenium deficiency, excess copper, and the thyroid peroxidase (TPO) Arg386His polymorphism, especially with the histidine/histidine genotype, are strongly associated with pediatric thyroid disease and high thyroid-stimulating hormone levels.
Meaning: Pediatric thyroid disorders are multifactorial. The TPO Arg386His variant may help identify children at higher risk of severe thyroid dysfunction, enabling earlier diagnosis, improved risk stratification, and more personalized clinical management.
- Pulmonology
- High-Risk CCL14 lineage drives severe Mycoplasma pneumoniae pneumonia in children: a study in central China
- Chunbo Hao, Zijie Li, Yanjuan Yu, Song Wang, Genhao Wang, Gaijing Jia, Tiantian Sun, Shouhang Chen, Yang Wu, Yu Tang, Fang Wang, Guangcai Duan, Yuefei Jin
- Clin Exp Pediatr. 2026;69(6):497-507. Published online April 10, 2026
-
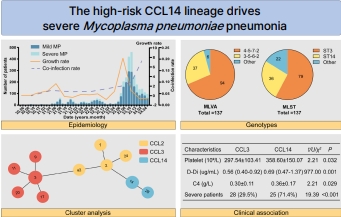
Question: Are the predominant circulating strains of Mycoplasma pneumoniae associated with disease severity and clinical indicators?
Finding: The common cluster label 14 (CCL14) lineage was a high-risk clone circulating in central China that demonstrated a strong association between severe pediatric pneumonia and a distinct hyperinflammatory profile.
Meaning: Targeted molecular surveillance of the CCL14 lineage may facilitate early risk stratification and guide clinical management to reduce the burden of severe disease.
- Endocrinology
- Anthropometric trajectories of Korean children and adolescents with severe obesity
- Jeongho Han, Hakyung Lee, Dong Jun Ha, Jieun Lee, Yong Hee Hong, Hwa Young Kim, Jaehyun Kim
- Clin Exp Pediatr. 2026;69(6):508-517. Published online April 10, 2026
-
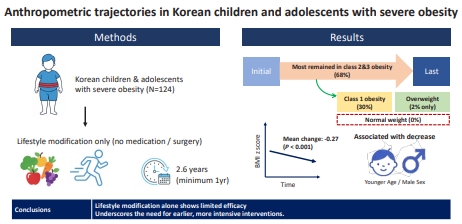
Question: How do body mass index (BMI) and metabolic markers change over time in severely obese Korean children and adolescents receiving only lifestyle modifications?
Finding: Among 124 participants, BMI z scores decreased modestly over 2.6 years, primarily in younger prepubertal boys. However, most remained severely obese, with minimal improvement in body composition or metabolic markers.
Meaning: Lifestyle interventions alone have limited efficacy for severe pediatric obesity. Early and more intensive treatments are required.
- Intramuscular and subcutaneous gonadotropin-releasing hormone agonist tests for central precocious puberty in girls: a randomized controlled trial
- Worapimon Lerdrassameethad, Suttipong Wacharasindhu, Vichit Supornsilchai, Khomsak Srilanchakon
- Clin Exp Pediatr. 2026;69(6):518-523. Published online April 15, 2026
-
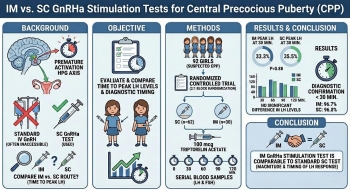
Question: Did the intramuscular (IM) and subcutaneous (SC) administration of gonadotropin-releasing hormone (GnRH) agonists have comparable timing and diagnostic utility for evaluating central precocious puberty in girls?
Finding: Both the IM and SC GnRH stimulation tests demonstrated comparable times to peak luteinizing hormone levels.
Meaning: Clinicians may consider the IM route as a time-efficient alternative, as it offers similar diagnostic utility for central precocious puberty without compromising the detection of hypothalamic-pituitary-gonadal axis activation.
- Clinical Note
- Gastroenterology
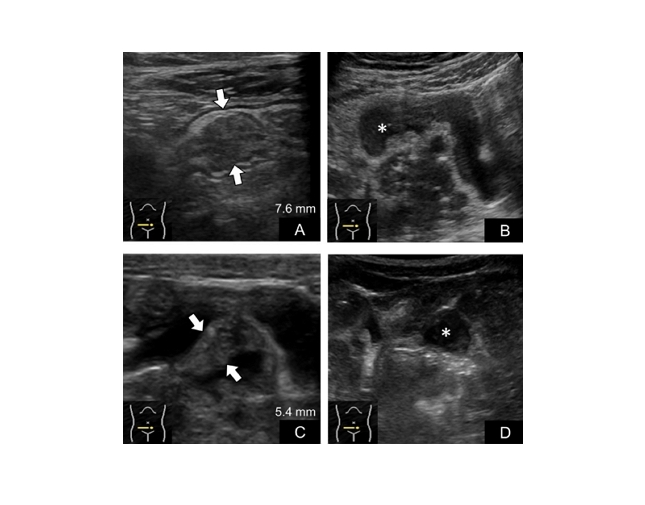
- Ultrasonographic features of 5-aminosalicylic acid intolerance in pediatric ulcerative colitis
- Hirotoki Murashige, Yasufumi Sakata, Yoshihiro Azuma, Shunji Hasegawa
- Clin Exp Pediatr. 2026;69(6):524-526. Published online May 28, 2026
-
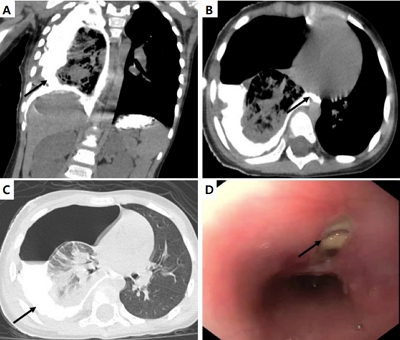
- Esophagopleural fistula following coin impaction in a female toddler: successful management using through-the-scope clips
- Sarthak Chakrabarti, Nikhil Sonthalia, Kaustabh Chaudhuri, Tamashis Mukherjee, Uday Chand Ghoshal, Mahesh Kumar Goenka
- Clin Exp Pediatr. 2026;69(6):527-530. Published online May 14, 2026
-