Article Contents
| Korean J Pediatr > Volume 60(11); 2017 |
|
Abstract
Purpose
The aim of this study was to investigate the statistical properties of four previously developed pediatric coronary artery z score models in healthy Korean children.
Methods
The study subjects were 181 healthy Korean children, whose age ranged from 1 month to 15 years. The diameter of each coronary artery was measured using 2-dimensional echocardiography and converted to the z score in the four models (McCrindle, Olivieri, Dallaire, and Japanese model). Descriptive statistical analyses and 1-sample t tests were performed.
Results
All calculated z scores had P values of ≥0.050 using the Kolmogorov-Smirnov test. The one sample t test showed that the mean z scores did not converge to zero except in 1 model, and the mean right coronary artery (RCA) z score was less than zero in all 4 models. The smaller RCA diameter in this study could be associated with the more distal measuring point used to avoid the conal branch. The percentage of subjects with extreme z score values (≥2.0 and ≥2.5) for the left main coronary artery (LMCA) seems to be higher in the Dallaire (4.9% and 3.3%) and Japanese models (7.1% and 3.8%).
Kawasaki disease (KD) is an acute, self-limiting febrile illness of unknown cause that affects the coronary arteries, predominantly occurring in children aged ≤5 years. KD was first described by Kawasaki in 19671) and is now known as the most common cause of acquired heart disease in children in developed countries2). The appropriate initiation of treatment with intravenous immunoglobulin reduces the incidence of coronary artery aneurysms from 25% to 4%3,4,5,6).
A quantitative assessment of the dimensions of the coronary artery using echocardiography is an important practice in the management of patients with KD. The criteria for coronary artery aneurysm, set by the Japanese Ministry of Health and Welfare in 1984, was a maximum internal diameter of ≥3 mm in children aged <5 years and ≥4 mm in children aged ≥5 years, a segment 1.5 times greater than the adjacent segment, and the presence of luminal irregularity7). Until recently, these criteria were widely used as they were easy to memorize and use. However, an underestimation of the incidence of coronary arterial lesions and an inability to reflect children's body growth in the application of these criteria have been pointed out8). A standardized score (z score) for assessing cardiovascular structures has been developed for use in pediatric clinical environments as children undergo rapid changes in their physical development with resultant variations in their body size9). Several coronary artery z score models have been subsequently proposed8,10,11,12,13,14,15); a relatively large number of subjects was included, and nonlinear regression methods were adopted in four of models12,13,14,15). In a recently published practice guideline by the American Heart Association, the classification of coronary arterial lesions is based on the z score of coronary artery diameter2). The previously reported z score model for Korean children has two major limitations: firstly, the number of subjects included in the study for the model was too small and secondly, a linear regression was adopted for model fitting of the body surface area16). The z score model by Kobayashi et al.15), which was derived from the lambda-mu-sigma method in 3,851 Japanese children, holds promise for use in Korean children due to its large sample size and the racial similarity between the Japanese and Korean populations.
In this study, an investigation of the statistical properties of 4 previously developed pediatric coronary artery z score models, including the Japanese model, was performed in relation to 181 healthy Korean children. We expected the results of this investigation to present useful information on the selection of z score models in clinical practice in Korea.
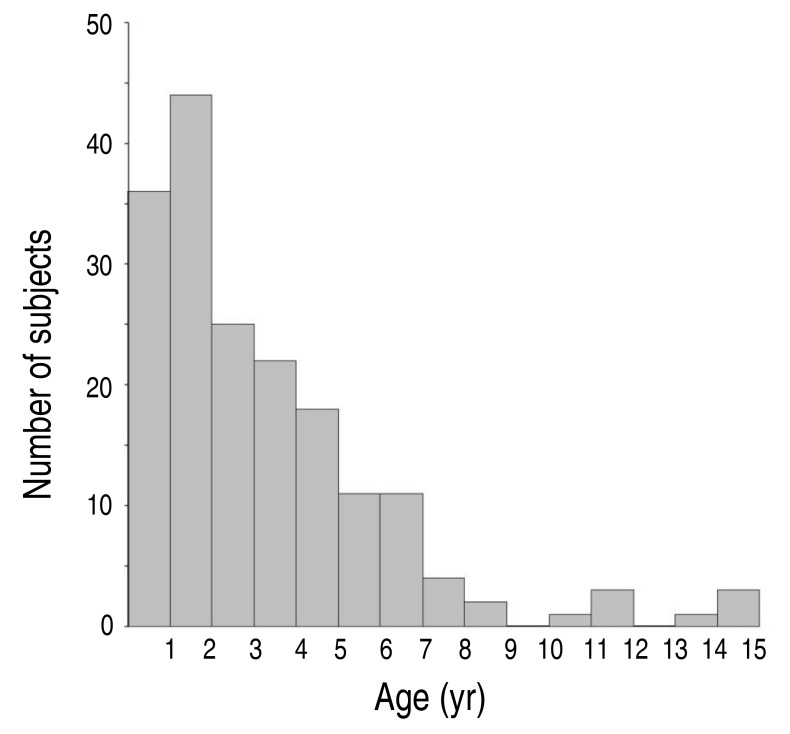
The study subjects were 181 healthy Korean children, whose ages ranged from one month to 15 years (Fig. 1), and who presented at the Asan Medical Center for an evaluation of a cardiac murmur, abnormal findings on chest radiography (e.g., borderline heart size), syncope, or transient chest pain. Echocardiographic studies showed no significant anatomical and functional abnormalities in the subjects. The subjects' demographic characteristics were evaluated through a review of their medical records. A body surface area was estimated using the Haycock formula17).
This study was approved by the Institutional Review Board of Asan Medical Center (2017-0853), and the requirement for informed patient consent was waived.
The standard method of measuring the diameter of coronary arteries in a pediatric population was applied according to the recommendation by the American Society of Echocardiography18). The intraluminal diameter of the coronary artery segments was measured from the inner to inner edges. The left main coronary artery (LMCA) was measured midway between the ostium and the bifurcation of the circumflex artery and the left anterior descending coronary artery (LAD) in the parasternal short-axis view. The LAD was measured distally to the bifurcation and before the start of the first marginal branch. A measurement for the right coronary artery (RCA) was obtained in the relatively straight section, just after the initial rightward turn from the anterior-facing sinus of the Valsalva. In a case with a visible origination of the conal branch, the RCA segment distal to the conal branch was measured (Fig. 2). The offline measurement of coronary artery diameters was performed by one author (JJY). The reproducibility of coronary artery diameter measurements has already been reported in another study which was performed by same echocardiographers19) (an intraobserver variability in the measurement of the LMCA, LAD, and RCA as 5.4%, 8.7%, and 5.1%, respectively, and the interobserver variability as 5.8 %, 10.4%, and 7.0%, respectively).
The diameters of each coronary artery were measured and converted to the z score using the previously reported regression equations or spreadsheet file for calculation12,13,14,15). The results of the z score of coronary artery diameter were analyzed using the Kolmogorov-Smirnov test on a normal distribution and using the 1-sample t test on a convergence of the average value to zero. Statistical analysis was performed using IBM SPSS Statistics ver. 21.0 (IBM Co., Armonk, NY, USA). Statistical significance was defined as P<0.05.
One hundred eighty-one children were included in the study, 47% of whom were male (Table 1). The age of subjects was median 2.34 years (range, 1 month to 15 years; Fig. 1). The weight of the subjects was median 12.6 kg (range, 2.9–73.9 kg) and the height was median 89.0 cm (range, 48.7–176.6 cm). The body surface area was median 0.559 cm2 (range, 0.201–1.909 cm2). The median diameter of LMCA, LAD, and RCA was 2.13 mm (range, 1.35–4.01 mm), 1.65 mm (range, 1.10–3.26 mm), and 1.60 mm (range, 0.82–3.65 mm), respectively (Table 1).
By definition, the z score values must be normally distributed and the mean value should converge to zero, the standard deviation to 1, the skewness to zero, and the kurtosis to zero. The descriptive statistical characteristics of the z score value is presented in Table 2 and plotted as a histogram in Fig. 3, 4, 5. The mean value of the z score of the RCA was less than zero in all 4 models. The values of skewness and kurtosis of the LMCA were above zero in all models. The P value on the Kolmogorov-Smirnov test for the z score value was ≥0.050 in three coronary arteries in all four models, which suggests the statistical feasibility of normal distribution. One sample t test showed that the mean z score value was significantly different from zero (Table 3); the only exception was a z score of the LAD in the Japanese model (P=0.582).
The percentage of subjects with a z score of the LMCA ≥2.0 in the Dallaire and Japanese models appears higher (4.9% and 7.1%, respectively) than 2.3% which is the proportion of the z score ≥2.0 in standard normal distribution (Table 4). Moreover, the percentage of the z score of the LMCA ≥2.5 also appears higher (3.3% and 3.8%, respectively) than 0.6% which is the proportion of the z score ≥2.5 in standard normal distribution in those 2 models. The extremely high z score of the LMCA seems to be more frequent in the Dallaire and Japanese models than in the other 2 models.
In this study, the descriptive statistical analyses of coronary artery diameter z scores in 181 normal children were performed using four frequently used z score models (Table 5)12,13,14,15). As all models are designed to represent a normal population, we expected that the calculated z scores for healthy children would also follow a normal distribution. The Kolmogorov-Smirnov test showed P≥0.050 in three coronary arteries in all 4 models, implying the statistical feasibility of normal distribution. Therefore, it was consequently estimated that the four z score models would be distributed normally, which justifies the application of these models to Korean pediatric populations.
We additionally expected that the mean value of the z score should converge to zero since the subjects were normal healthy children. However, the mean z score value of the 3 coronary arteries was significantly different from zero in each of the four models, except for one of the LADs in the Japanese model. The limited number of subjects in this study could be one of causes. Another explanation for this difference could be the subtle differences in the measuring points. In this study, the mean z score of the RCA was consistently less than zero in all models, which implies that the measured RCA diameters were smaller than the reference values of the z score models. It is reported in the z score model reference papers that the RCA measurements were obtained 2–5 mm distal to its origin in the parasternal short-axis view13,14,15). In this study, the RCA segment distal to the conal branch was measured in a case with a visible origination of the conal branch to avoid an exaggerated measurement on the branching point. In addition, the measurement point was more distal to 5 mm from the origin of the RCA in some of such cases. As a result, the RCA diameters in this study would have been smaller accordingly. We think that more precise instructions are needed for an accurate and reproducible measurement of the RCA proximal diameter on the issue of the conal branch.
Among the four z score models, the Dallaire and Japanese models were more favorably recommended for use in recent American Heart Association guidelines because they included a relatively larger number of subjects and provide normative data on the left circumflex branch2). Incidentally, the percentage of subjects with an extreme z score of the LMCA appears to be higher in the Dallaire and Japanese models in this study than the expected level under normal distribution. This higher percentage could be due to anatomic variation in several cases, which can be seen in the histograms for the LMCA (Fig. 3). The positive skewness and kurtosis in the distribution of the LMCA z score would not impact on the higher percentage of subjects with extreme z scores of the LMCA. It is well known that anatomic variations are frequent in the LMCA2). Additionally, caution in the interpretation of the LMCA z score was also recommended in recent guideline2). For the other branches of coronary arteries, all four z score models could reasonably be used for the evaluation of vascular dilatation.
The relatively small number of subjects is a limitation of this study.
In conclusion, all 4 models showed statistical feasibility of normal distribution. More precise instructions are needed for RCA measurement. A higher percentage of extreme z scores of the LMCA is compatible with a commonsense understanding of anatomic variations of the LMCA.
Notes
Conflicts of interest:
No potential conflict of interest relevant to this article was reported.
References
1. Kawasaki T. Acute febrile mucocutaneous syndrome with lymphoid involvement with specific desquamation of the fingers and toes in children. Arerugi 1967;16:178–222.

2. McCrindle BW, Rowley AH, Newburger JW, Burns JC, Bolger AF, Gewitz M, et al. Diagnosis, treatment, and long-term management of Kawasaki disease: a scientific statement for health professionals from the American Heart Association. Circulation 2017;135:e927–e999.


3. Suzuki A, Kamiya T, Kuwahara N, Ono Y, Kohata T, Takahashi O, et al. Coronary arterial lesions of Kawasaki disease: cardiac catheterization findings of 1100 cases. Pediatr Cardiol 1986;7:3–9.


4. Newburger JW, Takahashi M, Burns JC, Beiser AS, Chung KJ, Duffy CE, et al. The treatment of Kawasaki syndrome with intravenous gamma globulin. N Engl J Med 1986;315:341–347.


5. Dajani AS, Taubert KA, Takahashi M, Bierman FZ, Freed MD, Ferrieri P, et al. Guidelines for long-term management of patients with Kawasaki disease. Report from the Committee on Rheumatic Fever, Endocarditis, and Kawasaki Disease, Council on Cardiovascular Disease in the Young, American Heart Association. Circulation 1994;89:916–922.


6. Durongpisitkul K, Gururaj VJ, Park JM, Martin CF. The prevention of coronary artery aneurysm in Kawasaki disease: a meta-analysis on the efficacy of aspirin and immunoglobulin treatment. Pediatrics 1995;96:1057–1061.



7. Japan Kawasaki Disease Research Committee. Report of subcommittee on standardization of diagnostic criteria and reporting of coronary artery lesions in Kawasaki disease. Tokyo: Ministry of Health and Welfare, 1984.
8. de Zorzi A, Colan SD, Gauvreau K, Baker AL, Sundel RP, Newburger JW. Coronary artery dimensions may be misclassified as normal in Kawasaki disease. J Pediatr 1998;133:254–258.


9. Epstein ML, Goldberg SJ, Allen HD, Konecke L, Wood J. Great vessel, cardiac chamber, and wall growth patterns in normal children. Circulation 1975;51:1124–1129.


10. Kurotobi S, Nagai T, Kawakami N, Sano T. Coronary diameter in normal infants, children and patients with Kawasaki disease. Pediatr Int 2002;44:1–4.


11. Tan TH, Wong KY, Cheng TK, Heng JT. Coronary normograms and the coronary-aorta index: objective determinants of coronary artery dilatation. Pediatr Cardiol 2003;24:328–335.


12. McCrindle BW, Li JS, Minich LL, Colan SD, Atz AM, Takahashi M, et al. Coronary artery involvement in children with Kawasaki disease: risk factors from analysis of serial normalized measurements. Circulation 2007;116:174–179.


13. Olivieri L, Arling B, Friberg M, Sable C. Coronary artery Z score regression equations and calculators derived from a large heterogeneous population of children undergoing echocardiography. J Am Soc Echocardiogr 2009;22:159–164.


14. Dallaire F, Dahdah N. New equations and a critical appraisal of coronary artery Z scores in healthy children. J Am Soc Echocardiogr 2011;24:60–74.


15. Kobayashi T, Fuse S, Sakamoto N, Mikami M, Ogawa S, Hamaoka K, et al. A new Z score curve of the coronary arterial internal diameter using the Lambda-Mu-Sigma method in a pediatric population. J Am Soc Echocardiogr 2016;29:794–801.


16. Yu JJ, Cho SK, Park YM, Lee R, Chung S, Bae SH. Coronary artery diameter of normal children aged 3 months to 6 years. Korean J Pediatr 2008;51:629–633.

17. Haycock GB, Schwartz GJ, Wisotsky DH. Geometric method for measuring body surface area: a height-weight formula validated in infants, children, and adults. J Pediatr 1978;93:62–66.


18. Quiñones MA, Otto CM, Stoddard M, Waggoner A, Zoghbi WA. Doppler Quantification Task Force of the Nomenclature and Standards Committee of the American Society of Echocardiography. Recommendations for quantification of Doppler echocardiography: a report from the Doppler Quantification Task Force of the Nomenclature and Standards Committee of the American Society of Echocardiography. J Am Soc Echocardiogr 2002;15:167–184.


Fig. 2
Schematic representation of the locations used for coronary artery diameter measurement. RCA, right coronary artery; LMCA, left main coronary artery; LAD, Left anterior descending coronary artery; PA, pulmonary artery.
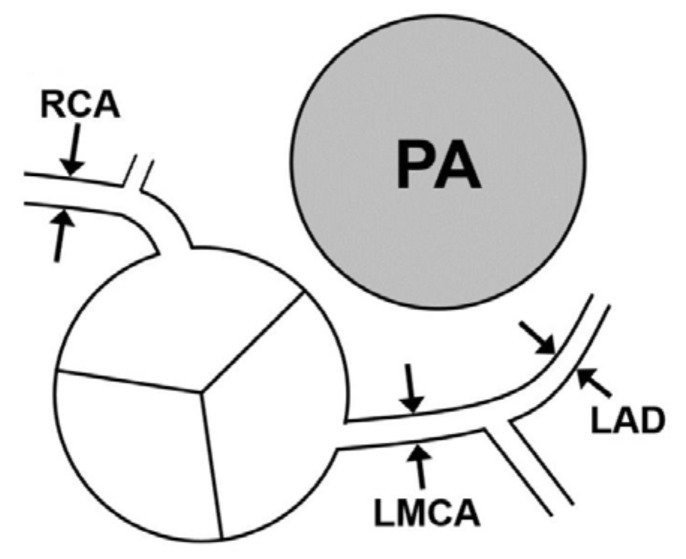
Fig. 3
Histograms for left main coronary artery z scores. (A) McCrindle model, (B) Olivieri model, (C) Dallaire model, and (D) Japanese model. SD, standard deviation.
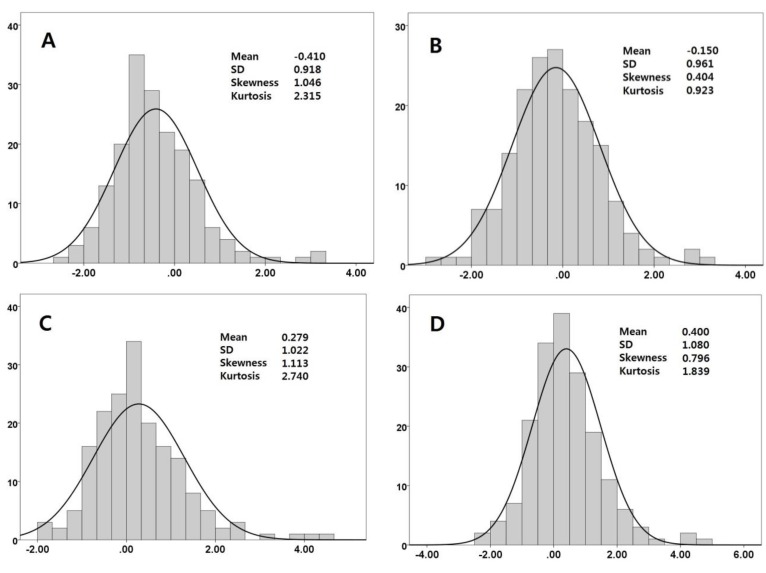
Fig. 4
Histograms for left anterior descending coronary artery z scores. (A) McCrindle model, (B) Olivieri model, (C) Dallaire model, and (D) Japanese model. SD, standard deviation.
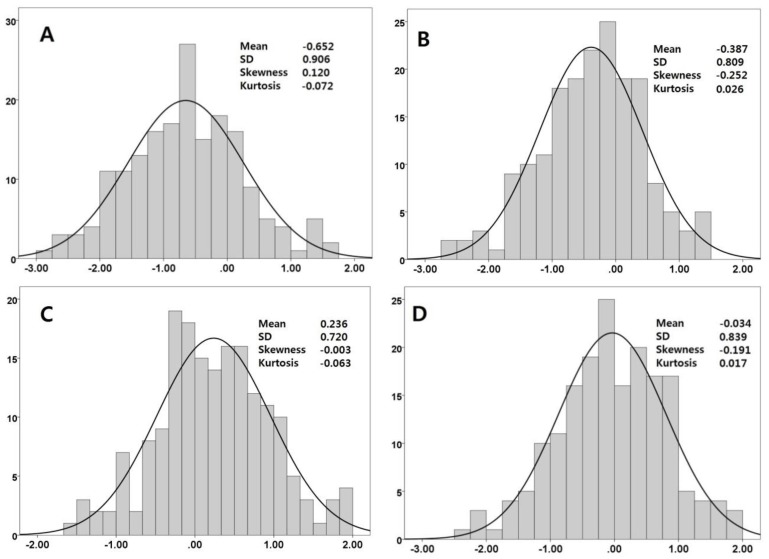
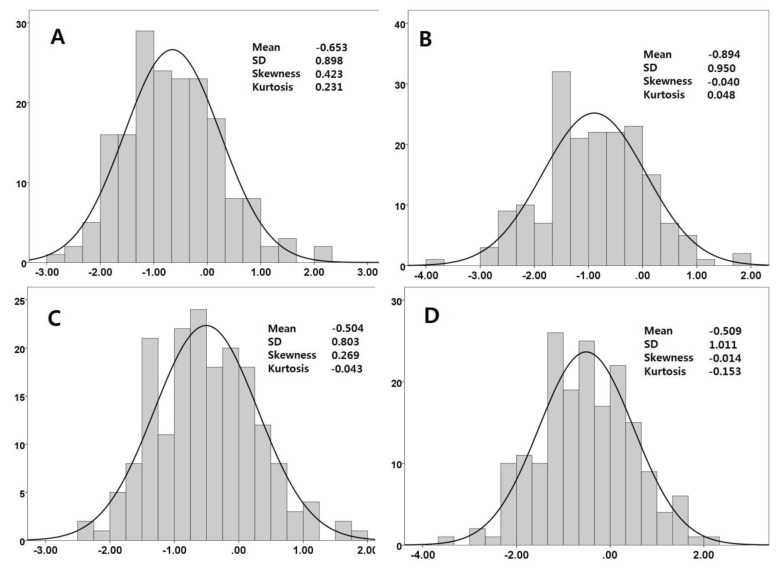
Fig. 5
Histograms for right coronary artery z scores. (A) McCrindle model, (B) Olivieri model, (C) Dallaire model, and (D) Japanese model.



 PDF Links
PDF Links PubReader
PubReader ePub Link
ePub Link PubMed
PubMed Download Citation
Download Citation


